|
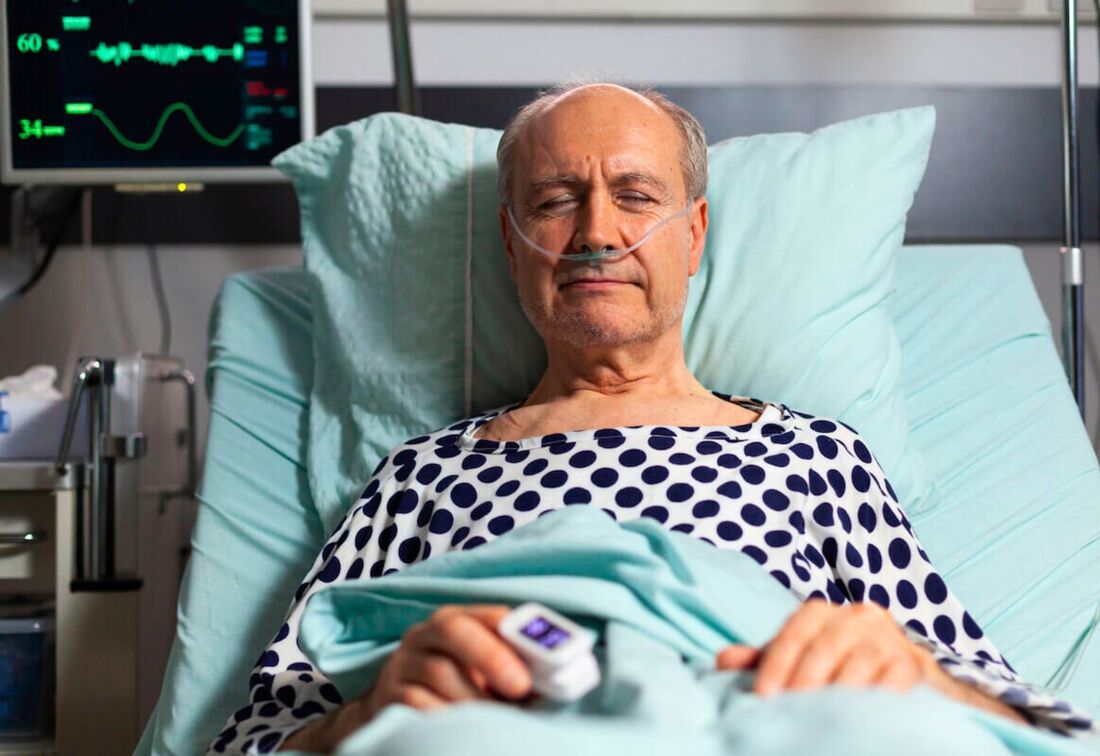
The demographic landscape of Malaysia is undergoing a significant transformation. The Department of Statistics has estimated that Malaysians aged over 65 will constitute 7.4 percent of the country's total population this year. This figure is projected to double in two decades and exceed 20 percent by 2056, effectively making Malaysia a super-aged nation. In response to this demographic shift, the government is planning to introduce a Mental Capacity Act for Malaysia in 2024, according to Deputy Minister in the Prime Minister’s Department (Law and Institutional Reform), M Kulasegaran.
The urgent need for the Mental Capacity Act The proposed Mental Capacity Act (MCA) aims to allow individuals to prepare for the management of their affairs in the event they become mentally incapacitated. By appointing trusted individuals or entities, people can ensure their matters are taken care of according to their wishes, even if they lose the ability to make decisions themselves. This legislative move is crucial in filling a significant void in Malaysia's current legal framework. Under the existing Mental Health Act 2001, the Court can only establish committees to manage the affairs and estate of a mentally disordered person after the person has already become incapacitated. Similarly, the Powers of Attorney Act 1949 revokes any power of attorney once the person becomes mentally disordered or unsound, unless it is given for valuable consideration and expressed to be irrevocable. While the proposed legislation is highly anticipated, it is still in its initial stages, and no specific timeframe has been set for when it will be tabled before the Malaysian Parliament. Deputy Minister M Kulasegaran stated that the government will engage with stakeholders to discuss the proposal, and a policy paper will be presented to the Malaysian Cabinet for approval before the drafting of the Act begins. He expressed hope that the policy paper could be tabled within this year. Insights from the APHM’s 30th International Healthcare Conference At the Association of Private Hospitals, Malaysia (APHM)’s 30th International Healthcare Conference and Exhibition, themed "Shaping the Future of Healthcare: Trends and Insights for Tomorrow," a panel dialogue highlighted the importance of the Mental Capacity Act and regulations from a medical and legal perspective. The panel included Datuk Dr Kuljit Singh, President of APHM, Dr Ariffin Marzuki Mokhtar, Consultant Cardiothoracic Anaesthesiologist at University Sains Malaysia, Nurulhuda Mansor, Partner at Shearn Delamore & Co, Trevor Jason Mark Padasian, Partner at Skrine, and Ramakrishna Tharini, Partner at Ram & Low, moderated by Shanti Abraham, Founder of Shanti Abraham & Associates. The panel discussed various scenarios highlighting the dilemmas faced by doctors and hospitals when patients lack mental capacity. For instance, Datuk Dr Kuljit Singh shared a scenario where an elderly patient, who was of sound mind but had multiple medical issues, was admitted to the ICU. The patient's next of kin, as designated in a loose nomination process, controlled all decisions, leading to conflicts among siblings, especially those arriving from different parts of the world. Another scenario involved a patient who introduced a young woman as his next of kin. When the patient slipped into a coma, the young woman made all decisions on his behalf. Upon the patient's death, another woman appeared, questioning the young woman's authority, highlighting the lack of clear legal documentation and the difficulties faced by medical professionals in such cases. Advanced planning and legal precedents Trevor Jason Mark Padasian emphasized the importance of the proposed Mental Capacity Act in establishing and maintaining a register of long-lasting powers of attorney and appointing deputies to oversee the affairs of incapacitated individuals. This Act would ensure precedents are set, and expertise is guaranteed when individuals lose capacity. This advanced planning is vital for protecting the interests of those who can no longer make decisions for themselves. Ramakrishna Tharini highlighted the provision for advanced medical directives or advanced care directives within the mental capacity legislation. These directives allow individuals to make decisions about their future medical treatment while they still have the capacity. For example, an advanced medical directive, often referred to as a living will, can specify that a person does not want to be resuscitated if they suffer a cardiac arrest. In jurisdictions like the UK and Singapore, advanced refusals, such as do-not-resuscitate orders, are legally binding if executed properly. However, Ramakrishna explained that other forms of advanced directives, such as requests for specific treatments, are not legally binding but provide valuable guidance to medical professionals. He shared a compelling example from UK to illustrate the complexities of advanced directives. A young woman, a member of the Jehovah's Witness faith, had prepared an advanced directive stating she should not receive blood transfusions in the event of a medical emergency. Jehovah's Witnesses typically refuse blood transfusions on religious grounds. However, years later, the woman renounced her faith and reverted to her original beliefs. Despite her change in faith, the directive, which specified that it could only be revoked in writing, remained legally binding. When this case came before the court, it faced a significant dilemma. The advanced directive explicitly stated that she should not be transfused and included a clause that it could only be removed in writing. Nevertheless, the court decided that, due to her change in circumstances and renouncement of her former faith, the doctors were permitted to administer a transfusion. This decision highlighted that legal safeguards exist to ensure that advanced directives are not only followed to the letter but also take into account the patient's likely wishes at the time of the medical decision. The importance of clear guidelines and carer support Nurulhuda Mansor noted that the Mental Capacity Act would provide clear guidelines on when a person lacks capacity and the roles and responsibilities of various parties involved in decision-making. This structure is essential for avoiding conflicts and ensuring that decisions are made in the best interest of the incapacitated individual. The Act would also offer guidance to carers and practitioners on their roles, helping them make informed decisions without bearing the full weight of responsibility. In Singapore, the code of practice supplements the Mental Capacity Act, serving as a day-to-day guidebook for carers and doctors. Balancing health and wealth considerations Datuk Dr Kuljit Singh emphasized the importance of considering both health and wealth in the context of an aging population. Advanced medical instructions should include components such as limits on medical expenses, indicating when to transfer from private to government hospitals. This planning can help manage costs and ensure that resources are used effectively. Learning from other jurisdictions Malaysia can learn from the experiences of other jurisdictions like the UK and Singapore, which have successfully implemented mental capacity legislation. These frameworks provide a clear definition of capacity, guidelines for decision-making processes, and the roles of various parties involved. As Malaysia prepares to address the challenges of an aging population, the introduction of the Mental Capacity Act is a crucial step towards ensuring that individuals' affairs are managed according to their wishes, even if they lose the ability to make decisions themselves. The Act will provide clear guidelines and support for carers and medical professionals, helping to avoid conflicts and ensure the best interests of incapacitated individuals. As we move towards implementing the Mental Capacity Act, we must ask ourselves: Are we prepared to support our aging population with the necessary legal and medical frameworks to ensure their dignity and wishes are respected in their most vulnerable moments? |
- IN THE SPOTLIGHT
-
HEALTH CONDITIONS
- ANTIMICROBIAL RESISTANCE
- ARTHRITIS
- ASTHMA
- BACK PAIN
- BRAIN DISORDERS
- BREAST CANCER
- CANCER
- CARDIOVASCULAR DISEASE
- CERVICAL CANCER
- CORONAVIRUS DISEASE (COVID-19)
- DEMENTIA
- DENGUE
- DENTAL PROBLEMS
- DIABETES
- DRUG ABUSE
- ECZEMA
- EPILEPSY
- EYE
- FIBROIDS
- GASTROINTESTINAL DISEASES
- INFLUENZA (FLU)
- HEADACHES & MIGRAINES
- HEPATITIS
- HIV & AIDS
- JOINT PAIN
- KIDNEY DISEASE
- LUNG CANCER
- LUPUS
- MELASMA
- MENTAL HEALTH
- MOUTH-AND-TEETH
- OBESITY
- OSTEOPOROSIS
- OVARIAN DYSFUNCTION: UNDERSTANDING PREMATURE OVARIAN FAILURE, POLYCYSTIC OVARY DISEASE AND INFERTILITY
- SEXUAL & REPRODUCTIVE HEALTH
- SKIN CONDITIONS
- SLEEP
- STROKE
- DISABILITIES & SPECIAL ABILITIES
- NURSING RESOURCES
- DIGITAL HEALTH
- HEALTH PRODUCTS & SERVICES
- RELATIONSHIPS
- FAMILY HEALTH & PARENTING
- EMPOWERING WOMEN
- MEN'S WELLNESS
- GOLDEN YEARS
- ACTIVE LIFE HUB
- NUTRITION
- COMPLIMENTARY MEDICINE
- HUMANITARIAN & COMMUNITY HEALTH
- AMBULANCE AND FIRST AID GUIDE
- Community clinics/ Klinik Komuniti
- Government Dental Clinics / Klinik Pergigian Kerajaan
- ABOUT US