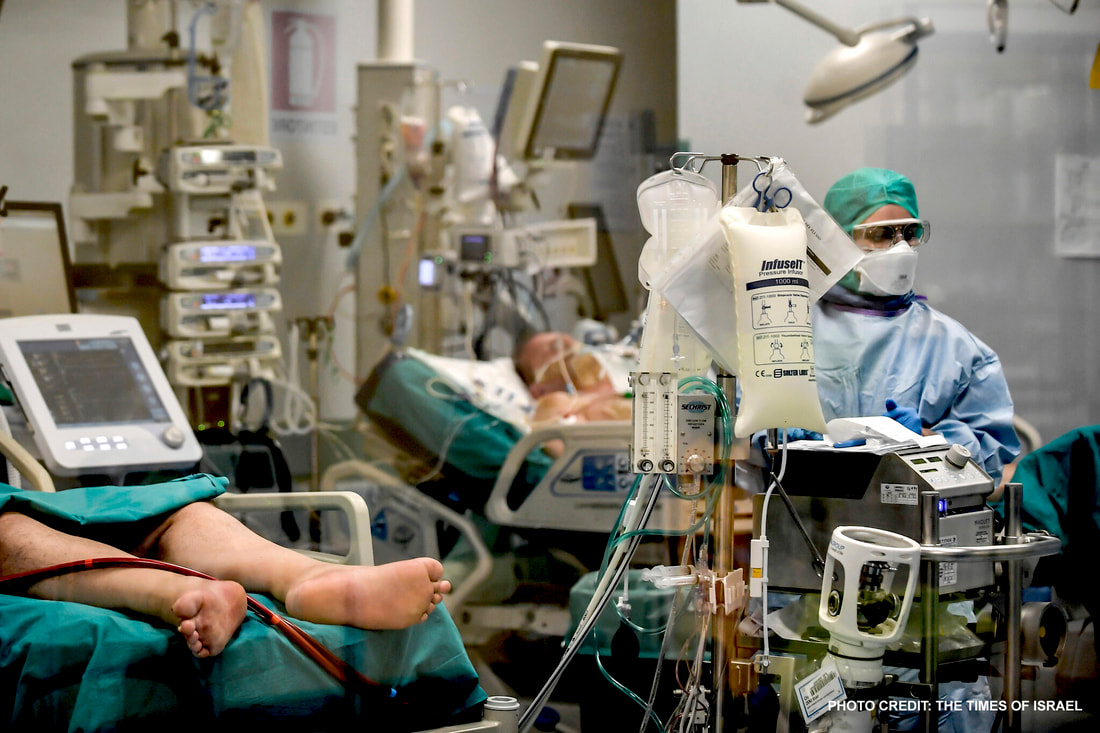
COVID-19: The legal implications of patients' lack of honesty
MAY 12, 2020 @ 4.30PM
Five doctors and nurses were infected with Covid-19 in Albania and more than 20 others were self-quarantined after they contracted the virus from patients they were treating who reportedly hid their recent travel history.
In neighbouring Thailand, 112 medical staff at the Vachira Phuket Hospital were suspended from work and placed in quarantine after the Hungarian tourist they were treating for an accident died of Covid-19 on April 3. The deceased had earlier withheld details of his visits to Soi Bangla – an entertainment area in tambon, Patong which is the epicentre of coronavirus transmission in Phuket. In both cases, patients refusal to be forthcoming with information is the likely cause of infection and the emergence of new cases. This beckons us to ask if more could be done to legally compel patients to be more forthcoming with critical information required by healthcare officials? Can Covid-19 patients be held liable if their action or inactions result in others getting infected? Duty of candour Duty of candour is commonly associated with the duty on the part of the health care provider – to be candid or open when an adverse event or error has been committed in the treatment of a patient. “That duty of candour or duty to be open in Malaysia on the part of the medical practitioners is an ethical duty that is codified in the Malaysian Medical Guidelines by the Malaysian Medical Council,” explains Raja Eileen Soraya Raja Aman, Partner at Raja, Darryl & Loh. “Unlike some jurisdictions like the United Kingdom, where they have a specific act or statute passed by Parliament - imposing that duty as a legal or as a statutory duty - in Malaysia however, arguably we don’t have such a legal duty. We don’t have a statutory duty imposed on medical professionals in relation to the duty of candour. There is however a clear ethical duty. What about the reverse situation? Is there a corresponding duty on the part of patients towards doctors and healthcare professional ? Patients need to be honest There is judicial recognition that patients need to be forthcoming with their health care providers. We see that for example in cases where – when patients are not forthcoming about their medical history and perhaps omit certain information; that has then resulted in some adverse outcome and the treatment being compromised because that health care professional simply did not have that information prior to starting the treatment. “We then have an adverse event. In such cases, the judiciary will consider the facts and the law. This can result in the health care professional being able to use that omission or failure to be forthcoming by the patient as a defence or shield, and in some cases as a complete defence if sued or a claim is made. “The argument is that – if I’m not told something and as a result, the treatment wasn’t successful – then the cause of the treatment being made unsuccessful - is not because of me as a health care provider that has actually done something wrong - but it’s because the patient had omitted certain information. So, that is a complete defence. “ It can also be a partial defence. The argument is that when there is a failure to be honest – that failure has contributed to the injury and hence there are concepts like ‘contributory negligence’. “This is well recognized and I am talking about normal circumstances – not necessarily during the Covid-19 period – so the duty to be honest is already there,” adds Raja Eileen. What about Covid-19 or pandemics of these kind? How would this duty fare? Speaking about the Prevention and Control of Infectious Diseases Act 1988 (PCIDA), Raja Eileen said that the Act has expressed provisions that make it mandatory for individuals to notify / to disclose information requested. “Regulations 2020 that were issued under this Act have made it compulsory for individuals to be honest and forthcoming with information when requested or otherwise face penal consequences. “In the current situation, we are looking at statutory obligations that are imposed by the Act. If we look at Section 10, the requirement to notify is not limited to the individual who may be infected or persons who feels he/she maybe infected, but that obligation extends to other occupants in a household. “So, it goes beyond the infected individual. Occupants of a household also have the obligation to notify. “The law is not unreasonable. If we look at the provision, it does say that the obligation is only imposed on an adult occupant of a particular household as soon as the person becomes aware of the existence of the disease with the least practicable delay. Those are the words that we find in this statute. Hence, if you’re completely unaware of an infected person in your household, who comes in and out and does not talk to you, you don’t see him or her, it doesn’t trigger the provision. Withholding information If a patient is infected or there is information that suggests that he/she may have come in close contact with an infected person, that person should try not to put other persons in harm’s way. “This applies to a health care provider who may be regarded as a vulnerable person when treating a patient who has an infection. Extra care has to be given due to the close proximity of that health care provider to the particular individual. As such, the quick answer as to whether you may sue a patient if the patient withholds material information that may harm a healthcare provider, is that an argument may be made, that you may. While she strongly discourages this, she pointed out several HIV cases in America and in England where suits have been instigated by individuals who were infected by someone already diagnosed or a person who was reckless and did so deliberately. So, the cause of action is there and is recognized. On April 13, Omar Mat Khatib, 31 was sentenced to three months community service by the Magistrate Court in Alor Setar, Kedah for concealing his travel history to health officer Mohamad Syazwan Mohd Esa. The first to be charged in Malaysia, the postman with Singapore Post Limited pleaded guilty to violating Regulating 6 of the Prevention and Control of Infectious Diseases (Measures within the Infected Local Areas) Regulations 2020 on March 26 at the Pendang district health clinic’s Covid-19 screening counter. |
EXPLORE FURTHER
Pharmacy cautions against self-medication and self-dosing of 'Ivermectin' to treat COVID-19No human use of Ivermectin is approved or registered in Malaysia
|
Could a single dose of the drug Ivermectin stop the SARS-COV-2 virus from growing?Ivermectin removed all viral RNA by 48 hours
|
Is it sinusitis or Covid-19?How COVID-19 symptoms differ from sinusitis: Key insights
|
The Malaysian response to Covid-19: Building preparedness for ‘surge capacity’, testing efficiency and containmentEarly coordination key to Malaysia's COVID-19 response success
|
Road to recovery: Care after COVID-19Understanding post-acute Sequelae of SARS-CoV-2 infection in patients
|
Covid-19: The legal implications of patients' lack of honestyHow can we legally encourage patients to share critical information?
|